By Anna Tullgren | Individual, Community & Challenge Event Fundraiser
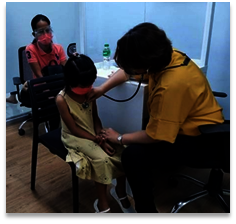
Thank you so much for your kind support of World Child Cancer’s project in the Philippines, where we are working to improve the diagnosis, access to treatment and quality of care for children with cancer on the island of Mindanao.
World Child Cancer's work in the Philippines has continued, improving access to, and quality of, childhood cancer services. This is vital as, when we started work on Mindanao in 2014, there was just one main medical centre able to diagnose and treat childhood cancer – the Southern Philippines Medical Centre (SPMC), which meant very poor access for children with cancer in the more remote areas. Travel across the island to reach treatment was extremely time-consuming and expensive for families, and a key factor in the poor diagnosis rates of just 15% of the 1,200 children expected to develop cancer each year. Our programme, working in partnership with lead Paediatric Oncologist from SPMC, Dr Mae Dolendo, is capacity-building the five Shared Care Centres so that they may take on more complex childhood cancer cases – this is done by providing mentorship and training in childhood cancer diagnosis and management for the medics at the Shared Care Centres.
Although face-to-face training was put on hold due to the COVID-19 pandemic and resulting lockdowns and restricted travel, we are delighted to report that Dr Dolendo’s visits to the facilities were able to resume this year. During these visits, Dr Dolendo met with key medical and hospital management staff to discuss and provide support on childhood cancer cases, as well as to advocate for increased provision of dedicated paediatric oncology nurses and staff.
It is thanks to supporters like you that so much recent progress towards improving children’s cancer services long-term has been made in Mindanao, and nationally. Thank you again for all your support.
Thank you for helping to give children with cancer the gift of growing up!
Links:
By Anna Tullgren | Individual, Community & Challenge Event Fundraiser
By Anna Tullgren | Individual, Community & Challenge Event Fundraiser
Project reports on GlobalGiving are posted directly to globalgiving.org by Project Leaders as they are completed, generally every 3-4 months. To protect the integrity of these documents, GlobalGiving does not alter them; therefore you may find some language or formatting issues.
If you donate to this project or have donated to this project, you can receive an email when this project posts a report. You can also subscribe for reports without donating.