By Sheena Millapo | Programme Officer
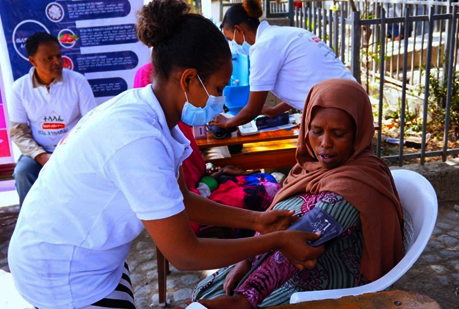
In quiet neighbourhoods across Ethiopia, something transformative has been unfolding, conversations about health are now taking place in people’s homes, on their doorsteps. Our project, “Improving NCD Care for Underserved Communities”, has been working at the grassroots to tackle the growing burden of non-communicable diseases (NCDs), particularly hypertension and diabetes. With the support of our trained Health Extension Workers (HEWs), we launched an intensive door-to-door campaign various members of the community. The initiative focused on raising awareness, offering screenings, and linking those found at risk to nearby clinics for timely care and follow-up.
These home visits did more than identify health concerns, they also empowered community members with essential knowledge. Individuals were sensitised on the risk factors and prevention of NCDs through direct engagement with HEWs, using verbal communication and simple visual aids. This personal approach helped to build trust, address misconceptions, and encourage lifestyle changes such as increasing physical activity and monitoring blood pressure regularly. Educational materials were distributed later at community events to reinforce these health messages in a setting where people could engage with the content more thoroughly.
The campaign has also played a key role in strengthening the link between communities and the local health system. By equipping HEWs with the tools to assess, inform, and refer individuals, and by ensuring these referrals are followed through at health facilities, we have laid a foundation for long-term, sustainable care. Through your giving, our work continues to highlight how personalised, community-based interventions can bring health services closer to people, making care not just accessible, but trusted and understood.
By Sheena Millapo | Programme Officer
By Sheena Millapo | Programme Officer
Project reports on GlobalGiving are posted directly to globalgiving.org by Project Leaders as they are completed, generally every 3-4 months. To protect the integrity of these documents, GlobalGiving does not alter them; therefore you may find some language or formatting issues.
If you donate to this project or have donated to this project, you can receive an email when this project posts a report. You can also subscribe for reports without donating.
Support this important cause by creating a personalized fundraising page.
Start a Fundraiser