

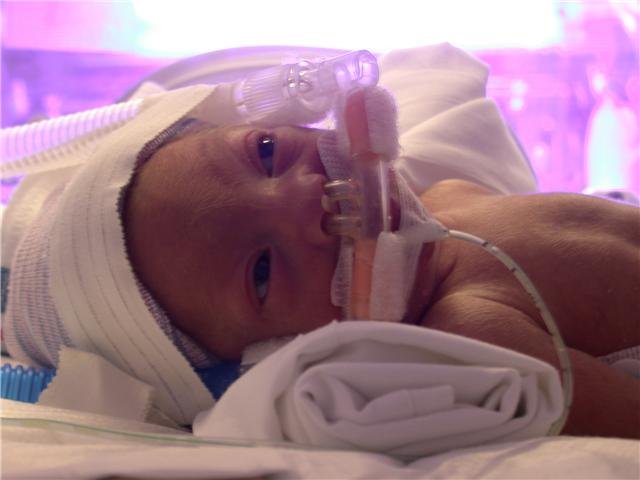

AIW is dedicated to recruiting qualified nurses to provide loving homes, nursing care, and other needed services for medically fragile foster care infants and children. We help facilitate the child's move from hospitals, group homes and institutions into private residences under the care of Registered and Licensed Vocational Nurses as their foster parents. We provide two essential ingredients for these children to heal - loving home environments and individualized nursing care.



Each of GlobalGiving’s nonprofit partners is required to send quarterly donor reports detailing the impact of their work. Here are some of their recent updates:
By Linda West-Conforti RN | Founder
Our Back Story: Nurse Linda West-Conforti, RN, new medically fragile foster child's divinely orchestrated foreseeing words shattered nurse Linda's complacency several decades ago and led to her... Read the full report ›By Linda West-Conforti RN | Founder
Our Back Story: Nurse Linda West-Conforti, RN, new medically fragile foster child's divinely orchestrated foreseeing words shattered nurse Linda's complacency several decades ago and led to her life's... Read the full report ›By Linda West-Conforti | Founder
Our Back Story: Nurse Linda West-Conforti, RN, new medically fragile foster child's divinely orchestrated foreseeing words shattered nurse Linda's complacency several decades ago and led to her life's... Read the full report ›