By Annie Niland | Community Giving Coordinator
As Haiti experiences on going civil unrest, Partners In Health is working tirelessly to keep our doors opened for patients. Staff are working long hours, scrambling to secure fuel for generators. Some have traveled hours by foot or motorcycle, dodging stones and tear gas, as they pass barricades to arrive for shifts. They are doing whatever it takes to take care of patients. We’re able to do this because of your partnership.
Madeleine was one among thousands of Haitians across the country caught in life-threatening situations, as Haiti continues to be mired in more than one month of protests that have resulted in some 200 people injured and 20 killed. Roadblocks and demonstrations have cut off transportation in and around the capital, as well as across the country, as inflation spikes and Haitians struggle to access gas, food, and clean water. Banks, schools, businesses, and many health care facilities have been closed for weeks. Yet Zanmi Lasante, as Partners In Health is known locally, has kept open all its clinics and hospitals at 12 sites across the lower Artibonite and Central Plateau, including University Hospital in Mirebalais.
On a Saturday in late September, the 33-year-old mother fell to the floor while trying to get into bed. Soon she began feeling pains and noticed fluid discharge, interpreting them as the signs of early labor. With growing concern, she called her physician, who informed her that no one was at the clinic to help. Demonstrations and barricades had blocked all traffic.
Madeline and her husband, Stevenson, were informed that University Hospital was still opened. They soon hired a taxi and made the would be 45-minute trip to the University Hospital. While in route to hospital, the couple would face road blocks and protesters. While explaining the situation of an expecting mother, the couple were allowed to pass through and directed to an unaffected route. Two hours after leaving their home, the couple reached their destination.
Nursing staff swung into action. Madeleine was suffering from pre-eclampsia, they realized, and needed immediate attention. While they worked to get her blood pressure under control, they prepared her for labor so that, late Sunday evening, she safely delivered two babies before midnight. Two more babies followed in the wee hours of Monday morning.
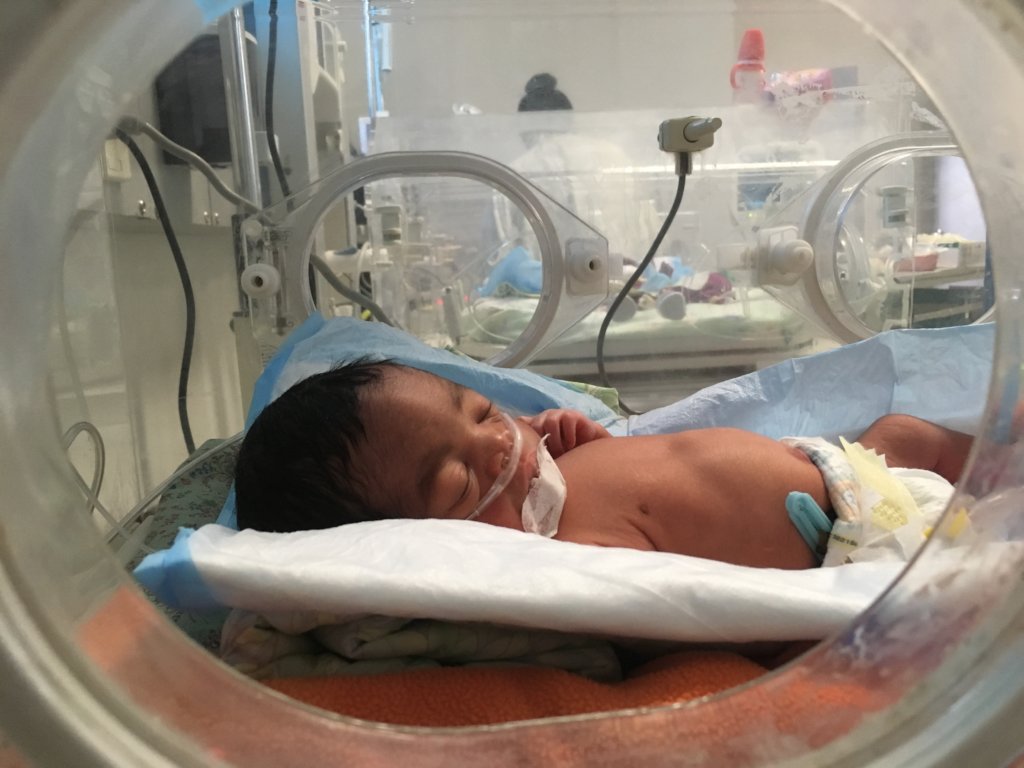
Two girls arrived at 2.5 and 3.4 pounds, and two boys at 3.6 and 4 pounds. Because the newborns were underweight and had arrived more than two months early, they were placed in incubators to maintain their body temperature and receive constant monitoring in the NICU. While waiting to be transferred, Stevenson provided one of the babies kangaroo care, which allows infants skin-to-skin contact with their caregivers to help maintain body heat and stimulate feeding.
Meanwhile, Madeleine was in critical condition herself. She had lost a good amount of blood and required a transfusion. Hearing that the unrest had momentarily calmed, hospital leadership sent an ambulance to the Red Cross in Port-au-Prince that Tuesday to gather lifesaving units of O+ blood. The driver arrived back, safe and sound, and staff immediately provided the new mom with a transfusion.
The family remains in good hands at University Hospital, where they are cared for by a rotating crew of Haitian clinicians who arrive for shifts after overcoming their own obstacles each day. PIH staff form the backbone of a hospital that is trusted and always open, with lights on to receive more patients, like Madeleine and her family, every day.
In Haiti, PIH remains the largest non-profit health care provider, and as such we will continue to work to provide the citizens with quality healthcare, reaching toward the ultimate goal of eliminating deaths and preventable illness. Your support has contributed to Madeline and children’s success as well as the thousands of lives that are impacted everyday through our organization. On behalf of our patients, staff and communities, we thank you!
Links:
By Victor Ukatu | Development Support Coordinator
By Victor Ukatu | Development Support Coordinator
Project reports on GlobalGiving are posted directly to globalgiving.org by Project Leaders as they are completed, generally every 3-4 months. To protect the integrity of these documents, GlobalGiving does not alter them; therefore you may find some language or formatting issues.
If you donate to this project or have donated to this project, you can receive an email when this project posts a report. You can also subscribe for reports without donating.