



Rotary is a volunteer organization of 1.2 million business, professional and community leaders united worldwide to provide humanitarian service. The mission is to enable Rotary's members to advance world understanding, goodwill and peace through the improvement of health, the support of education and the alleviation of poverty. Rotarians lead service programs in their communities and abroad that address today's most pressing challenges while encouraging high ethical standards in their vocations.




Each of GlobalGiving’s nonprofit partners is required to send quarterly donor reports detailing the impact of their work. Here are some of their recent updates:
By Amy Edwards | Program Specialist, PolioPlus
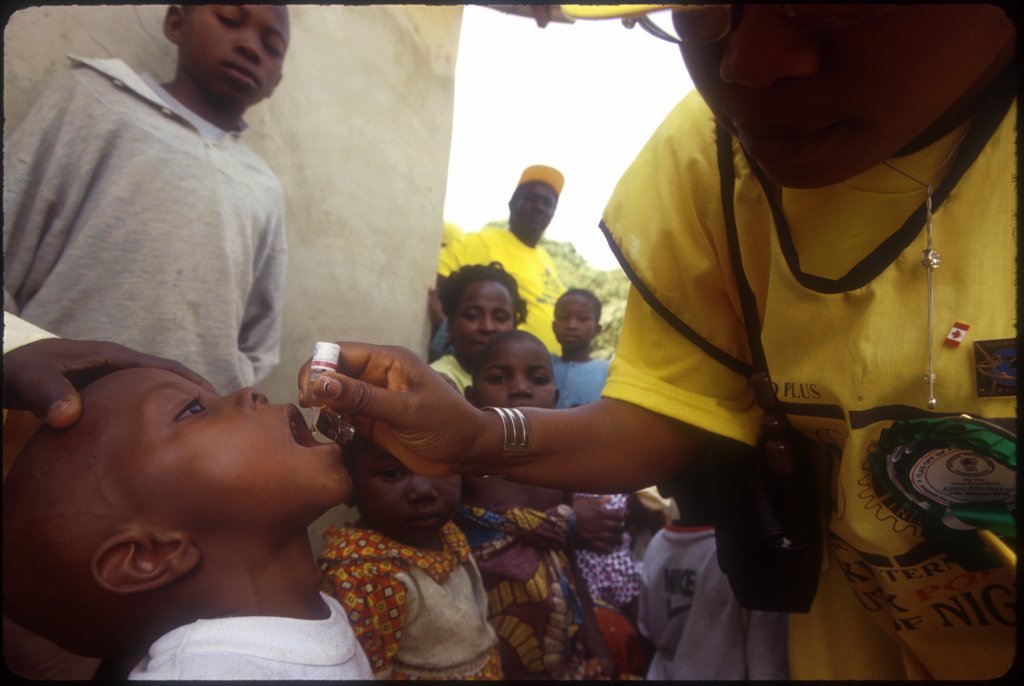
Committed to ensuring that every child is safe from the paralysis caused by poliovirus, Rotary International has donated a $ 14 million grant to the government of Nigeria to support polio surveillance... Read the full report ›By Amy Edwards | PolioPlus Program Specialist
Several African countries are considered at high risk for a polio outbreak. But for many years, Malawi wasn’t one of them. The nation has a sound public health infrastructure, and its... Read the full report ›By Amy Edwards | Program Specialist, PolioPlus
Health workers in Pakistan go door to door administering the polio vaccine. Volunteers in Zambia perform a dramatic skit showing how malaria spreads. These efforts may seem very different, but... Read the full report ›