



Our mission is to provide a preferential option for the poor in health care. By establishing long-term relationships with sister organizations based in settings of poverty, Partners In Health strives to achieve two overarching goals: to bring the benefits of modern medical science to those most in need of them and to serve as an antidote to despair. We draw on the resources of the world's leading medical and academic institutions and on the lived experience of the world's poorest and sickest communities. At its root, our mission is both medical and moral. It is based on solidarity, rather than charity alone. When our patients are ill and have no access to care, our team of health pr... read more Our mission is to provide a preferential option for the poor in health care. By establishing long-term relationships with sister organizations based in settings of poverty, Partners In Health strives to achieve two overarching goals: to bring the benefits of modern medical science to those most in need of them and to serve as an antidote to despair. We draw on the resources of the world's leading medical and academic institutions and on the lived experience of the world's poorest and sickest communities. At its root, our mission is both medical and moral. It is based on solidarity, rather than charity alone. When our patients are ill and have no access to care, our team of health professionals, scholars, and activists will do whatever it takes to make them well-just as we would do if a member of our own families or we ourselves were ill.






Each of GlobalGiving’s nonprofit partners is required to send quarterly donor reports detailing the impact of their work. Here are some of their recent updates:
By Kristen Jenkinson | Manager of Community Giving
On behalf of all our staff and patients, thank you for your generous giving to Partners In Health! We are so grateful for your partnership. The COVID-19 pandemic highlighted many opportunities for... Read the full report ›By Kristen Jenkinson | Manager of Community Giving
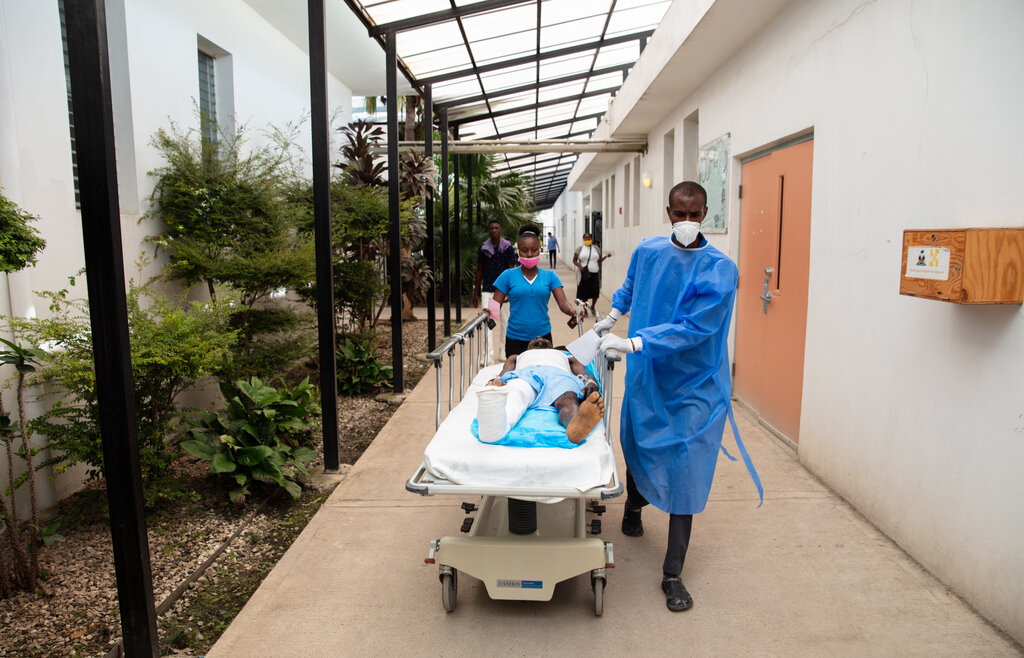
On behalf of all our staff and patients, thank you for your generous giving to Partners In Health! We are so grateful for your partnership. The cholera outbreak that struck Haiti threatened lives,... Read the full report ›By Kristen Jenkinson | Manager of Community Giving
On behalf of all our staff and patients, thank you for your generous giving to Partners In Health! We are so grateful for your partnership. The cholera outbreak that struck Haiti threatened lives,... Read the full report ›