By Ann Lolordo | Director of Communications
Afghan Health Providers’ Response to a Leading Cause of Deaths in Pregnant Women
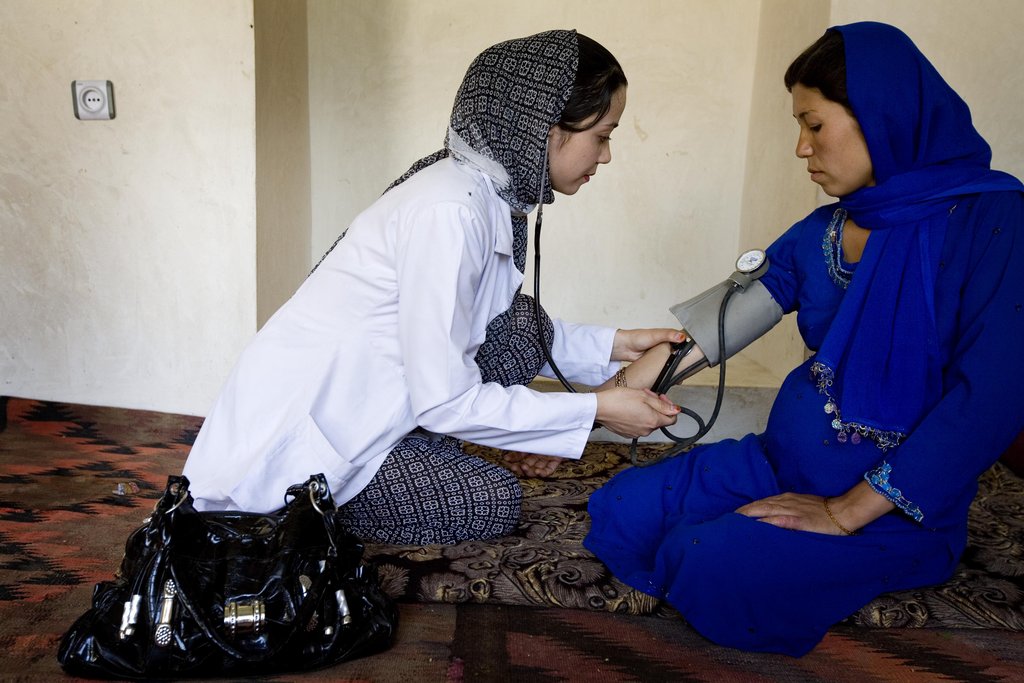
A leading cause of women dying in childbirth in the developing world is a pregnancy-related blood pressure condition known as pre-eclampsia/eclampsia. Symptoms of the potentially life-threatening condition of pre-eclampsia are elevated levels of protein in a pregnant woman’s urine and high blood pressure after 20 weeks. If undiagnosed and unmanaged, pre-eclampsia can rapidly progress to eclampsia (convulsions/fits)—the deadliest form of the condition. In Afghanistan, health statistics show that 20 percent of maternal deaths are the result of hypertensive conditions.
Midwives in Afghanistan who have been trained by Jhpiego have learned to screen for pre-eclampsia/eclampsia during prenatal visits and treat it appropriately. In an effort to ensure that Afghan midwives and their physician colleagues are delivering appropriate care, Jhpiego did an analysis of health care facilities that provide emergency obstetric and newborn care and their response to pre-eclampsia/eclampsia. Jhpiego-supported staff interviewed 224 health care providers at 78 facilities and found that all of the facilities had the proper equipment—blood pressure cuffs and stethoscopes—and three-fifths had urine test strips to check for high levels of protein in a pregnant woman’s urine. In addition, from 76.7 percent to 96 percent of these facilities had a complete IV set to maintain fluid balance and administer antihypertensives and magnesium sulfate, which has been shown to reduce the risk of death from eclampsia by 45 percent.
As to the competency of health care providers, the analysis showed that 96 percent of doctors and 89 percent of midwives recognized that magnesium sulfate should be used to manage severe pre-eclampsia/eclampsia, but 42 percent of doctors and 58 percent of midwives also thought another drug, diazepam, had a role to play in treating these women. Diazepam is recommended when magnesium sulfate is not available. While supplies of anticonvulsant drugs were available at the facilities, the drugs weren’t always used, according to the analysis.
These findings suggest a need to clarify service delivery guidelines, offer refresher training and bolster best practices with supervision and reinforcement for health care providers, especially for those working in facilities with fewer women presenting with symptoms of pre-eclampsia/eclampsia.
According to the journal article on the analysis results mentioned above, “The study findings will be used to help inform continuing education and reinforcement efforts in Afghanistan and also to standardize supplies and equipment across different facility levels. More broadly, they can contribute to the development of effective strategies for translating health worker knowledge into practice in low-income countries.”
By Carolyn McKenna | Director, Individual Donors
By Ann Lolordo | Director, External Relations and Communications
Project reports on GlobalGiving are posted directly to globalgiving.org by Project Leaders as they are completed, generally every 3-4 months. To protect the integrity of these documents, GlobalGiving does not alter them; therefore you may find some language or formatting issues.
If you donate to this project or have donated to this project, you can receive an email when this project posts a report. You can also subscribe for reports without donating.